management of portal

Management of portal
hypertension, BuddeChiari
syndrome and portal vein
thrombosis
Andrew K Burroughs
Abstract
The risk of variceal bleeding can be estimated by the size of varices, the
presence of endoscopic red signs and the degree of liver dysfunction. All
patients with large varices, and those with cirrhosis and severe liver
disease, irrespective of the size of varices, should be given primary prophy-
laxis with non-selective b-blockers. Banding ligation is equivalent and is
used if there are contraindications or intolerance to these drugs. Acute var-
iceal bleeding should be managed in a gastrointestinal bleeding unit.
Prophylactic third-generation cephalosporins and vasoactive drugs should
always be given. Ligation or sclerotherapy should take place at diagnostic
endoscopy. Secondary prophylaxis of variceal bleeding is mandatory with
combined b-blockers and ligation. Hepatic outflow obstruction syndromes
have a wide spectrum of presentation. Underlying thrombophilic condi-
tions should be sought. A fulminant presentation requires liver transplan-
tation. Decompression with transjugular intrahepatic stent shunt is
effective in many cases and can also be used in cases of portal vein throm-
bosis. Hepatic and other venous webs can be treated with interventional
radiological techniques. Anticoagulation is first-line therapy and should
be continued lifelong; it should also be used in non-cirrhotic portal vein
thrombosis, and considered in cirrhotic portal vein thrombosis.
Keywords antibiotics; anticoagulation; BuddeChiari syndrome; hepatic
venous outflow syndromes; ligation of varices; portal hypertension;
portal vein thrombosis; propranolol; terlipressin
In severe chronic liver disease, the principal problems are:
the degree of hepatocellular failure
the complications of portal hypertension.
Portal hypertension and gastrointestinal bleeding
Risk of variceal bleeding
1
In cirrhotics with oesophageal varices that have not bled, the risk
of bleeding is related to the:
size of the varices (tension on the vessel wall is greater, for
the same pressure, in a larger vessel than in a smaller vessel)
presence of red signs at endoscopy (red weal marks)
degree of liver dysfunction.
It is likely, but not proven, that these risk factors also apply to
non-cirrhotic portal hypertension. The risk factors for gastric
variceal bleeding are unknown.
Varices bleed from the lower 5 cm of the oesophagus, just above
the oesophagogastric junction. The mechanism of bleeding is
explosive, caused by high pressure, rather than erosive as a result
of reflux of gastric acid. If varices have bled, the risk of rebleeding
is at least 70%; there is only a modest association between the risk
of rebleeding and the degree of liver dysfunction. At admission up
to 50% of patients have culture-positive sepsis.
Management of acute bleeding episodes
Admission to hospital: any patient with melaena or haematem-
esis should be admitted to hospital, particularly if chronic liver
disease is suspected, and managed by a joint medicalesurgical
team (preferably part of a gastrointestinal bleeding unit), with
intensive nursing care.
Initial assessment eclinical and laboratory evidence of the
severity of bleeding and the degree of liver dysfunction and
infection must be sought on admission, because all have prog-
nostic significance. The following should be evaluated:
haemoglobin/haematocrit, white blood cell count, platelet
count
serum urea and electrolytes, and creatinine
prothrombin and partial thromboplastin times
baseline liver function tests
blood and urine cultures
ascitic tap
chest radiograph
ECG
blood gases (in patients with decompensated cirrhosis or
suspected chest disease).
What’s new?
CIn acute variceal bleeding, antibiotics should always be used as
they reduce early rebleeding and mortality eintravenous third-
generation cephalosporins are effective. Transjugular
intrahepatic stent shunt (TIPSS) improves survival when used
as first-line therapy in patients unlikely to respond to endo-
scopic methods. Removable oesophageal covered stents stop
bleeding, and are also an option in this group of patients.
Injection of adhesive glues are particularly effective for acutely
bleeding gastric varices
CFor primary prophylaxis of variceal bleeding, non-selective
b-blockers are the first-line treatment option
CIn secondary prophylaxis against variceal rebleeding, combined
banding ligation and non-selective b-blockers is the most
effective treatment
CTIPSS with covered stents have greatly improved patency rates
and are part of the treatment algorithms for gastric variceal
bleeding, BuddeChiari syndrome (BCS) and portal vein
thrombosis (PVT)
CAnticoagulation is first-line therapy in BCS and non-cirrhotic
PVT, followed by radiological intervention. The risk of further
thrombosis outweighs the risk of bleeding. The evidence in
favour of anticoagulation in PVT with cirrhosis is less robust
Andrew K Burroughs MBChB Hons FEBG FRCP FMedSci is a Consultant
Physician and Hepatologist and Professor of Hepatology at the Royal
Free Hospital and University College London, London, UK. Competing
interests: none declared.
MANAGEMENT PROBLEMS IN LIVER DISEASE
MEDICINE 39:10 607 Ó2011 Elsevier Ltd. All rights reserved.

The presence of any of the following indicates a poor prognosis:
jaundice
ascites
encephalopathy
low serum albumin
prolonged prothrombin time
raised serum creatinine
shock or low haemoglobin on admission
infection and other concomitant disease.
Initial therapy: is aimed at correcting hypovolaemia, stopping
the bleeding, and preventing the complications of gastrointes-
tinal bleeding and deterioration of liver function.
1
Hepatic
encephalopathy and fluid retention should be treated and pre-
vented by standard methods. Potassium canrenoate can be given
intravenously as a substitute for oral spironolactone. To prevent
sodium overload, sodium chloride infusions should not be used
and strict attention must be given to electrolyte balance.
Prophylactic antibiotics (oral quinolones) are mandatory. If
sepsis is either suspected or obviously present, the most suitable
‘blind’ treatment is a third-generation cephalosporin (e.g. cefo-
taxime), depending on nosocomial bacterial resistance profiles;
nephrotoxic antibiotics must be avoided. The use of antibiotics
from admission reduces early rebleeding and improves
survival.
1e3
Alcohol withdrawal problems must be anticipated. Intrave-
nous benzodiazepines are suitable sedatives, but should be
monitored carefully and titrated for their sedative effect. In
patients with symptoms of alcohol withdrawal, adequate treat-
ment is required before endoscopy. All alcoholics should be
given intravenous thiamine preparations on admission. Enteral
and, occasionally, parenteral nutrition should be administered to
patients with poor nutrition, when bleeding has been controlled.
Vitamin K
1
, 10 mg intravenously (IV) should be given routinely.
There is no evidence that gastric acid suppression is benefi-
cial, but intravenous or oral ranitidine should be given when the
bleeding is caused by a gastric mucosal lesion.
The target haemoglobin concentration for transfusion should
be 8 g/dl as this reduces the chances of early rebleeding.
1
Endoscopy: should be performed only when resuscitation has
been achieved. Nasal oxygen should be given and pulse oximetry
measured. If sedation is required, endoscopy should be per-
formed under a brief general anaesthetic.
1
Visualization of the portal anatomy and liver: should be under-
taken early, particularly when hepatocellular carcinoma is sus-
pected or the patient is a candidate for surgery or a transjugular
intrahepatic stent shunt (TIPSS). Ultrasonography and echo
Doppler ultrasonography should exclude an obvious space-
occupying lesion and establish the patency of the portal and
hepatic veins. It may be difficult to obtain good views; retrograde
CO
2
portography (Figure 1) or splanchnic arteriography with views
of the venous phase may be necessary to visualize the portal vein.
Vasoactive drugs: are given on the suspicion of portal hyper-
tensive bleeding and before endoscopy as follows:
4
Terlipressin, 2 mg IV 6-hourly, is a synthetic analogue of
vasopressin (triglycyl lysine vasopressin) with intrinsic
vasoconstrictor activity and a longer duration of effect than
vasopressin because it is cleaved in the circulation. Terli-
pressin is contraindicated in ischaemic heart disease. The
ECG must be monitored during therapy.
Somatostatin and octreotide have almost no adverse effects.
Neither has more than a modest effect on portal pressure, but
they alter blood flow through varices. Somatostatin 250 mgbyIV
bolus followed by 250 mg/hour by infusion is superior to placebo
and has an efficacy similar to that of tamponade, terlipressin and
sclerotherapy. Octreotide (long-acting somatostatin) 50 mg/hour
acts similarly but there is far less evidence for its efficacy.
Vasopressin plus nitroglycerin, terlipressin and somatostatin are
less effective in decompensated cirrhosis. Only terlipressin has
been shown to increase survival compared with placebo. The role
of vasoactive drugs is therefore confined to adjuvant therapy or as
a ‘holding measure’ until more definitive therapy can be given.
Balloon tamponade: controls bleeding in more than 90% of patients.
Most tubes have four lumens to inflate the gastric balloon, inflate the
oesophageal balloon, aspirate the stomach, and aspirate above the
oesophageal balloon. The patient should, preferably, be intubated
before insertion. Balloon tamponade should be used to prevent
exsanguination when transfusion cannot match the blood volume
lost, and to enable safe transport of the patient to a referral centre.
Balloons should, ideally, remain in place for no more than 12 hours
(and certainly no more than 24 hours) to reduce the risk of local
mucosal ischaemic damage. A further endoscopic procedure (scle-
rotherapy, banding or glue injection) must be performed immediately
after the balloon has been removed, because the risk of rebleeding is
high. Another form of tamponade, which allows the patient to eat and
drink, is an expandable, covered and removable mesh metal stent,
which can be placed endoscopically or radiologically.
Emergency endoscopic techniques: sclerotherapy, banding
ligation, and injection of glue are the only methods that stop
active bleeding effectively in 85% of patients with variceal
bleeding.
1,4,5
All require expertise.
In sclerotherapy, sclerosant (5% ethanolamine in the UK) is
injected into and/or next to the variceal columns, 2e3 cm above
the oesophagogastric junction. A single injection session controls
bleeding in 70% of patients; in 85%, bleeding is controlled after
two sessions. The success of the procedure is related partly to the
severity of liver disease. Injection of 1% human thrombin or
cyanoacrylate glues is also effective. No benefit is gained by using
more than two injection sessions eTIPSS should be preferred.
Minor complications (e.g. retrosternal pain, fever, oesophageal
ulceration, sympathetic pleural effusion) are common, but major
complications (e.g. oesophageal perforation, mediastinitis,
venous embolization of sclerosant, infection) are rare.
Banding ligation places pre-stretched rubber bands on vari-
ceal columns using a delivery device mounted at the end of an
endoscope. It is slightly more effective than sclerotherapy and
has fewer complications, but requires double intubation so as
to load the banding device.
TIPSS: is placed radiologically. A transjugular approach is most
commonly used to enter the hepatic vein (Figure 2). It is
particularly useful for continued bleeding after endoscopic
therapy, and for gastric variceal bleeding.
6
It may have a role as
MANAGEMENT PROBLEMS IN LIVER DISEASE
MEDICINE 39:10 608 Ó2011 Elsevier Ltd. All rights reserved.

first-line therapy in selected patients at high risk of failing with
endoscopic methods. Portal vein thrombosis is not a contraindi-
cation and often can be resolved by TIPSS placement.
1,4
It is
available only in specialized centres. Patients should be referred
before the onset of severe infective or renal complications.
Surgery: TIPSS has replaced emergency surgery; oesophageal
staple-gun transection is rarely needed. Emergency shunts are
seldom used, as are devascularization procedures (if portal and
mesenteric thrombosis is present). Isolated splenic vein throm-
bosis is treated by splenectomy.
Prevention of rebleeding
The recommended therapy is combined banding ligation and
non-selective b-blockers.
1
Banding ligation: ligation of each varix is performed at 1e2-
week intervals. The aim is to obliterate the varices in the lower
oesophagus, resulting in a fibrosed oesophageal wall and/or
small thrombosed varices. Complications are less severe
following elective banding than after emergency banding, and
fatal complications are rare. In randomized studies, banding
ligation is more effective and safer than repeated sclerotherapy
and has replaced it.
Endoscopic follow-up should be undertaken every 3 months,
once the varices have been eradicated. If they reappear, they
should be treated again, as above. If varices have not reappeared
after 1 year, 6-monthly checks can be instituted; if no varices are
seen after 2 years, annual checks are sufficient.
Pharmacological therapy: non-selective b-blockers (e.g.
propranolol) lower pressure in the varices by reducing cardiac
output (b
1
-blockade), by allowing unopposed b-vasoconstriction
in the splanchnic bed (b
2
-blockade) and by a specific effect on the
collateral circulation. However, not all cirrhotic patients respond
and some do not tolerate b-blockade. When the hepatic venous
pressure gradient (HVPG) is reduced to 12 mmHg or less, or it falls
by at least 20% from baseline, the risk of rebleeding is very low and
other complications of cirrhosis are reduced. Non-selective
b-blockers are usually given in increasing daily doses to achieve
a resting pulse rate of 60 beats/minute or a maximal tolerance in
terms of hypotension or other collateral effects. Repeated portal
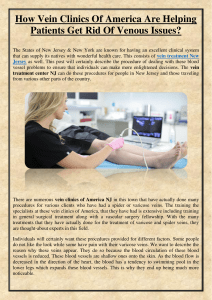
Figure 1 (a) Typical spider-web appearance on hepatic venography. (Note retrograde portal filling.) (b) Typical compression of intrahepatic inferior vena
cava. (Pressures e19 mmHg right atrium, 56 mmHg intrahepatic inferior vena cava, 38 mmHg intrahepatic inferior vena cava.) (c)CO
2
portogram (50 ml
injection) showing a fully patent portal vein in a cirrhotic patient just before insertion of a transjugular intraheptic portosystemic stent shunt. No
radiological dye is needed.
MANAGEMENT PROBLEMS IN LIVER DISEASE
MEDICINE 39:10 609 Ó2011 Elsevier Ltd. All rights reserved.

pressure measurements are invasive, but act as a ‘splanchnic
sphygmomanometer’
7
; their clinical applicability is debated.
8
Shunt surgery: with the advent of endoscopic therapy, surgery is
now a salvage procedure, particularly in patients who are not
candidates for transplantation. Major complications are operative
mortality, portosystemic encephalopathy and deterioration of
liver function caused by diversion of portal blood, which deprives
the liver of hepatotrophic factors and prevents ‘detoxification’ of
the portal blood. Use of small-bore 8-mm interposition H-graft
portacaval shunts reduces the incidence of encephalopathy.
Selective shunts (e.g. distal splenorenal shunt) also cause less
encephalopathy but this advantage is lost after 2 years.
4
Devascularization surgery: should be reserved for patients in
whom non-operative treatments have failed and who cannot
undergo shunt surgery or TIPSS. Transplant surgery is compli-
cated more by devascularization than by shunts as a result of the
formation of numerous adhesions, which contain portal hyper-
tensive collaterals that bleed extensively.
TIPSS: TIPSS using polyethylene-covered stents, maintain greater
patency and need far less re-intervention than the older ‘bare’
stents. Rebleeding rates are less than with endoscopic therapy,
but there is an increased risk of hepatic encephalopathy.
1
Primary prophylaxis for bleeding from varices
A non-selective b-blocker is the first choice, as these drugs
produce a statistically significant reduction in bleeding and
a trend towards reduced mortality. In cirrhosis, varices should be
evaluated endoscopically.
1
If there are no contraindications,
those with varices at risk of bleeding, including patients with
small varices and poor liver function, should be given b-
blockers.
1
Band ligation has been used in those with
contraindications or intolerance to b-blockers; survival is similar
and bleeding less but iatrogenic bleeding is reported. Prevention
of varices is not possible with non-selective b-blockers alone.
9
BuddeChiari syndrome
Aetiology and presentation
BuddeChiari syndrome is an obstruction of the major hepatic
veins.
10
The principal cause is thrombosis, caused by a thrombo-
philic disorder in 75% of patients. Primary myeloproliferative
disorders are most common, but all genetically based pro-
thrombotic tendencies (e.g. protein S or protein C deficiencies,
factor V Leiden, JAK2 mutations) can be a cause, particularly in
association with the oral contraceptive pill and puerperium.
Paroxysmal nocturnal haemoglobinuria and lupus anticoagulant
must also be considered.
The classical syndrome of ascites, hepatomegaly and abdominal
pain occurs with obstruction at any level of the hepatic venous
outflow tract, from the hepatic venule to the right atrium. ‘Hepatic
venous outflow block’ is the best term for these conditions.
Constrictive pericarditis should always be considered because it
mimics this presentation. An asymptomatic form is also recognized.
The rapidity and extent of thrombosis determines the severity of
congestion and necrosis spreading out from the central veins, and
thus the clinical presentation. A fulminant presentation caused by
massive ischaemic necrosis is indistinguishable from fulminant liver
failure. In chronic cases, the thrombosis is asynchronous, accounting
for atrophy and congestion of adjacent parts of the liver; fibrosis and,
eventually, cirrhosis supervene with chronic portal hypertension.
Classically, there is hypertrophy of the caudate lobe, which drains
directly into the inferior vena cava and often compresses it.
10
Diagnosis
The clinical background and an ascitic tap with a high protein
content should raise the possibility of BuddeChiari syndrome.
Doppler ultrasonography is usually sufficient to confirm the
diagnosis. The portal vein is also thrombosed in 10% of patients
and the inferior vena cava in 20%; thus, a detailed radiological and
haemodynamic assessment (including caval pressure measure-
ments above and below the liver) is needed. A typical ‘spider-web’
appearance on hepatic venography is diagnostic, and retrograde
CO
2
portography often outlines the portal vein (Figure 1). Minimal
use or avoidance of radiological contrast should be routine, to
minimize renal dysfunction.
10
Liver biopsy should be performed; it often shows diagnostic
features of centrilobular necrosis and sinusoidal congestion
(transjugular biopsy is often necessary but not always feasible).
It is useful to assess the degree of necrosis and fibrosis, but these
have minor prognostic value. Bone marrow examination and
chromosomal analysis are essential to assess the prognosis in
myeloproliferative disorders.
10
Screening for thrombophilic disorders (including screening of
relatives) must always be undertaken.
10
Management
The initial therapy is anticoagulation. If there is no improvement
further measures must be considered.
10
Shunts: management of BuddeChiari syndrome should, ideally,
be undertaken in a transplant centre because shunting can
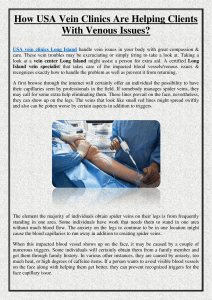
Intrahepatic stent shunt links the hepatic vein with the
intrahepatic portal vein. The hepatic vein is usually cannulated
via the transjugular route, through the heart.
Hepatic vein Right main portal
vein branch
Left gastric
vein
Metal expandable
stent covered with
polyethylene
Inferior
vena cava
Portal vein
Intrahepatic stent shunt
Figure 2
MANAGEMENT PROBLEMS IN LIVER DISEASE
MEDICINE 39:10 610 Ó2011 Elsevier Ltd. All rights reserved.

precipitate hepatic failure and transplantation is then an emer-
gency rescue procedure.
10
Early referral is essential.
Options for decompression with shunts are limited in patients
with thrombosis or severe compression of the inferior vena cava;
only a suprahepatic shunt (from splanchnic veins to the heart e
meso-atrial shunt) or TIPSS (which can be performed even in those
with obstructed hepatic veins) is suitable. Otherwise, TIPSS or a side-
to-side portacaval shunt is the procedure of choice. A surgical shunt
should not be used in patients who present acutely. A 95% 5-year
survival can be achieved in chronic cases. All forms of shunting
reduce hepatic parenchymal perfusion, so liver reserve and reversible
liver injury must be assessed to ensure adequate residual function.
Liver transplantation: is the preferred option when shunting is
impossible or fails; 5-year survival is 70% or more and it may be
the treatment of choice in fulminant cases.
11
Balloon dilatation: when isolated webs are found in the hepatic
veins and inferior vena cava (more common in the Far East),
balloon dilatation of these often relieves the obstruction.
10
Anticoagulation: should be used long term, particularly after
shunting and after liver transplantation, regardless of whether
a cause is found. Multiple thrombophilic risk factors may co-
exist, including as yet unidentified ones. Thrombolytic therapy
is not usually effective.
10
Portal vein thrombosis (PVT)
Aetiology and presentation
The causes are umbilical sepsis and any intra-abdominal sepsis
causing secondary thrombosis, and also carcinoma of the
pancreas and other malignancies.
12,13
Thrombophilic syndromes are the principal primary cause,
coagulation defects being more common than myeloproliferative
disorders. PVT can occur as a complication of cirrhosis in 0.6e16%
ethe most frequent causes are invasion by hepatocellular carci-
noma (HCC), as well as a pro-coagulant tendency in patients with
advanced cirrhosis and a decreased hepatopetal flow.
PVT is an adverse prognostic factor in cirrhosis, whether or
not associated with HCC.
12,13
Patients may be asymptomatic, with splenomegaly that is
either palpable or diagnosed incidentally by imaging, or may
present with bleeding from varices at the gastro-oesophageal
junction or further down the gastrointestinal tract, or rarely
with an acute abdomen due to mesenteric infarction.
Diagnosis
Ultrasound Doppler is the imaging modality of choice, followed
by cross-sectional CT or MRI with contrast, to diagnose associ-
ated malignancies and to define the extent of thrombosis.
A thrombophilia screen should be performed, as for BuddeChiari
syndrome, and relatives screened if this is positive.
12
Management
In the absence of malignancy in non-cirrhotic PVT, lifelong
anticoagulation should always be evaluated as first-line therapy,
as the risk of further thrombosis is substantially greater than that
of bleeding.
12
Many centres eradicate varices by ligation before
starting anticoagulation, whether or not there has been previous
bleeding. The evidence for benefit of anticoagulation in cirrhotic
PVT is less clear-cut; the risk and adverse consequences of var-
iceal bleeding are far greater than in those without cirrhosis.
12
Increasingly, anticoagulation is used for patients awaiting liver
transplantation as thrombotic extension into the superior
mesenteric vein may make the surgery impossible.
13
Bleeding gastro-oesophageal varices are treated as described
previously. PVT is not a contraindication to TIPSS, which is
successful in 65% of cases.
13
It can be used if bleeding is not
controlled by endoscopic methods, or when anticoagulation is
contraindicated, particularly before transplantation, although it
is preferable to anticoagulate after TIPSS to increase patency
rates. Thrombolytic therapy is rarely effective but has been used
in cases of very recent acute mesenteric infarction, or when
surgery for this complication is not possible.
12,13
A
REFERENCES
1de Franchis R, Baveno V Faculty. Revising consensus in portal
hypertension: report of the Baveno V Consensus Workshop on
methodology of diagnosis and therapy in portal hypertension.
J Hepatol 2010; 53: 762e88.
2Hou MC, Lin HC, Liu TT, Kuo BI, Lee SD. Antibiotic prophylaxis after
endoscopic therapy prevents rebleeding in acute variceal haemor-
rhage: a randomized trial. Hepatology 2004; 39: 746e53.
3Thalheimer U, Triantos CK, Samonakis DN, Patch D, Burroughs AK.
Infection, coagulation and variceal bleeding in cirrhosis. Gut 2005;
54: 556e63.
4de Franchis R, ed. Proceedings of the Fifth Baveno International
Consensus Workshop on methodology of diagnosis and treatment of
portal hypertension. Oxford: Blackwell Publishing, 2011.
5Triantos CK, Goulis J, Patch D, et al. An evaluation of emergency
sclerotherapy of varices in randomised trials: looking the needle in
the eye. Endoscopy 2006; 38: 797e807.
6Chau T, Patch D, Chan Y, Nagral A, Dick R, Burroughs AK. Salvage
transjugular portosystemic shunts egastric fundal compared with
esophageal variceal bleeding. Gastroenterology 1998; 114: 981e7.
7Abraldes J, Tarantino I, Turnes J, Garcia-Pagan J, Rodes J, Bosch J. Hae-
modynamic response to pharmacological treatment of portal hyperten-
sion and long term prognosis of cirrhosis. Hepatology 2003; 37: 902e8.
8Villaneuva C, Aracil C, Colomo JM, et al. Clinical trial: a randomized
controlled study on prevention of variceal rebleeding comparing
nadalol and ligation vs hepatic venous pressure gradient guided
pharmacological therapy. Aliment Pharmacol Ther 2009; 29: 397e408.
9Groszmann RJ, Garcı
´a-Tsao G, Bosch J, et al. Beta-blockers to prevent
gastro-oesophageal varices in patients with cirrhosis. N Engl J Med
2005; 353: 2254e61.
10 Senzolo M, Cholongitas E, Patch D, Burroughs AK. Update on the
classification, assessment of prognosis and therapy of BuddeChiari
syndrome. Nat Clin Pract Gastroenterol Hepatol 2005; 2: 182e90.
11 Mentha G, Giostra E, Majno PE, et al. Liver transplantation for
BuddeChiari syndrome: a European study of 248 patients from 51
centres. J Hepatol 2006; 44: 520e8.
12 Tsochatzis EA, Senzolo M, Germani G, Gatt A, Burroughs AK, et al.
Systematic review: portal vein thrombosis in cirrhosis. Aliment Pharmacol
Ther 2010; 31: 366e74.
13 Webster GJM, Burroughs AK, Riordan SM. Review article: portal vein
thrombosis enew insights into aetiology and management. Aliment
Pharmacol Ther 2005; 21: 1e9.
MANAGEMENT PROBLEMS IN LIVER DISEASE
MEDICINE 39:10 611 Ó2011 Elsevier Ltd. All rights reserved.
1
/
5
100%